Hormones
Brain Fog, Fatigue, Gut Issues: Why Perimenopause Starts in Your Gut
28 April 2026 · By Dr. B.J. Huber · 9 min read
You walk into the kitchen and forget why you’re there. A colleague’s name, someone you’ve worked with for years, just vanishes. By mid-afternoon your head feels foggy and heavy, you can barely string a thought together. Then there’s the bloating you never used to get, and a tiredness that a full night’s sleep does nothing for.
Most women in their early 40s put this down to stress, lack of sleep, or “just getting older.” Their doctor runs blood work, everything comes back normal. But something is clearly off. What often goes unnoticed is that these symptoms (brain fog, memory lapses, fatigue, digestive trouble) share a common root. And it sits somewhere most people wouldn’t think to look.
- Your estrobolome (estrogen-recycling gut bacteria) loses diversity during perimenopause, which accelerates hormonal decline from within the gut itself.
- 95% of your body’s serotonin is made in the gut. When microbial diversity drops, the pathway from tryptophan to serotonin falters, fueling brain fog and mood swings.
- The first human study on menopausal “gut leak” found that intestinal permeability measurably increases from pre- to postmenopause (Vieira et al., 2020).
Why does perimenopause actually begin in the gut?
Estrogen and the gut microbiome regulate each other in both directions. As estrogen drops during perimenopause, the gut flora shifts: beneficial species like Lactobacillus and Bifidobacterium decline while pro-inflammatory bacteria like Enterobacter gain ground. At the same time, the gut recycles less estrogen, which accelerates the hormonal decline even further.
That’s why classic perimenopause symptoms rarely show up alone. Brain fog, fatigue, and digestive issues are linked through three mechanisms, all of which start in the gut: the estrobolome, the gut-brain axis, and rising intestinal permeability.
What is the estrobolome and how does it amplify estrogen decline?
The estrobolome is a group of gut bacteria that produce the enzyme β-glucuronidase. This enzyme reactivates used-up estrogen in the intestine so it can re-enter the bloodstream, a process called enterohepatic circulation (Baker et al., 2017).
During perimenopause, this cycle comes under pressure from both sides. The ovaries make less estrogen, which reduces microbial diversity. Lower diversity means less β-glucuronidase, which means less estrogen gets recycled, which deepens the hormonal decline further. Data from the Hispanic Community Health Study showed that postmenopausal women had significantly fewer β-glucuronidase gene orthologs than premenopausal women, and that these changes tracked with worse cardiometabolic markers (Peters et al., 2022).
The bottom line: your gut isn’t a passive bystander during hormonal change. It either amplifies or buffers estrogen decline. To understand perimenopause, you have to start with the gut.
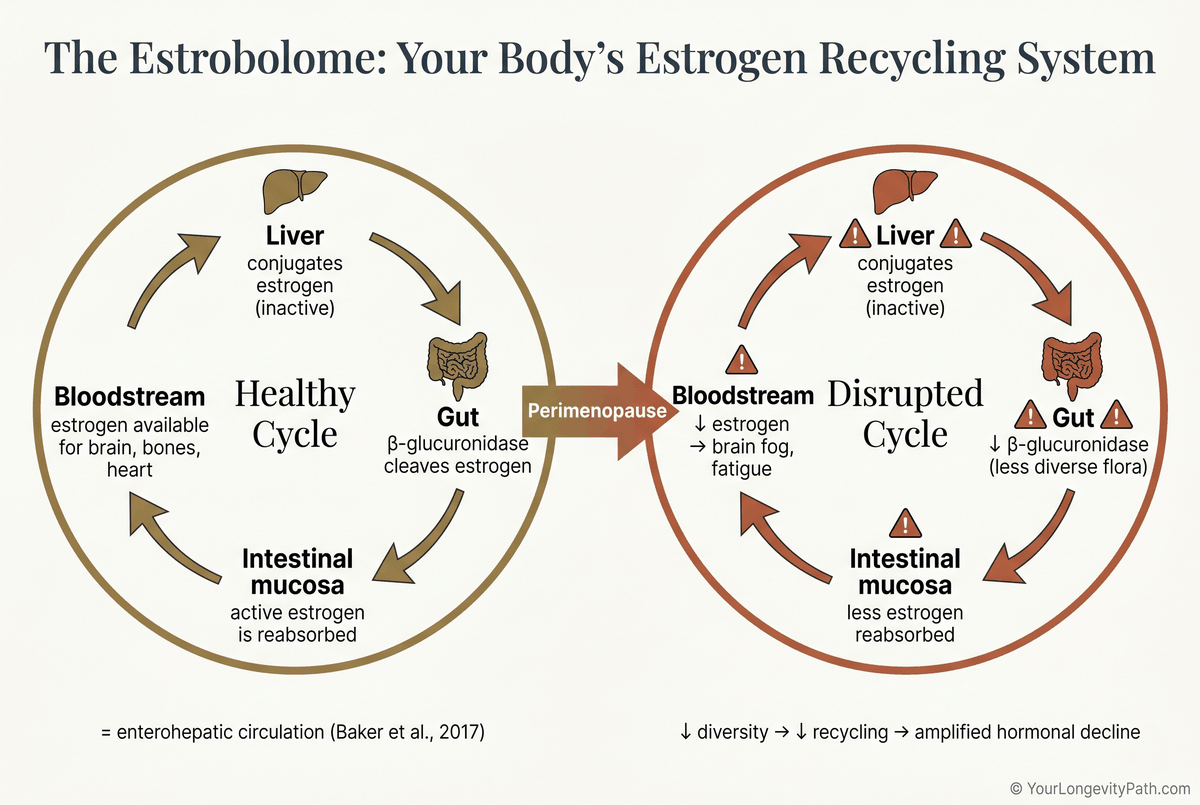 Fig. 1: The estrobolome recycles estrogen via the enterohepatic circulation. During perimenopause, microbial diversity declines, reducing β-glucuronidase production and amplifying hormonal decline (Baker et al., 2017; Peters et al., 2022).
Fig. 1: The estrobolome recycles estrogen via the enterohepatic circulation. During perimenopause, microbial diversity declines, reducing β-glucuronidase production and amplifying hormonal decline (Baker et al., 2017; Peters et al., 2022).
How are the gut-brain axis, serotonin, and brain fog connected?
About 95% of your body’s serotonin is made in the gut, not the brain. When microbial diversity drops during perimenopause, tryptophan metabolism shifts, serotonin production falters, and the result shows up as brain fog, mood swings, and trouble concentrating.
The gut-brain axis is a two-way communication line between the enteric nervous system and the central nervous system. It runs through the vagus nerve, the immune system, and microbial metabolites. During perimenopause, this axis gets hit on multiple fronts: microbiome diversity declines, Lactobacillus and other serotonin-associated bacteria drop off, and tryptophan increasingly converts into kynurenine instead of serotonin (Chen et al., 2025).
On top of that, another layer of protection falls away: estrogen directly supports serotonin production and tryptophan availability. There’s an energy angle too. The brain relies on estrogen (particularly estradiol) to convert glucose into fuel. When estrogen drops, neurons fire more slowly because they’re running on less energy. When both estrogen and microbial diversity decline at the same time, you get a serotonin deficit that shows up clinically as brain fog, poor concentration, and emotional instability. Epperson and colleagues (2011) showed that serotonin plays a critical role in verbal working memory and emotion processing during menopause.
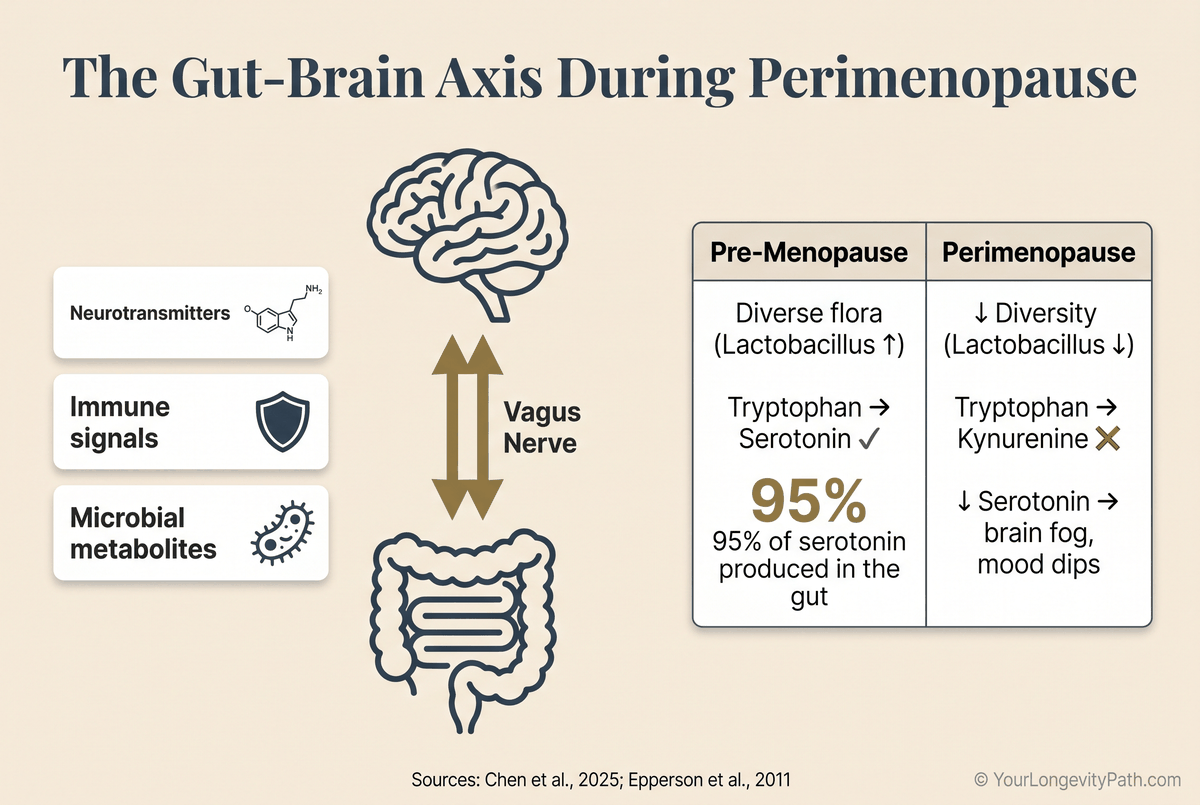 Fig. 2: 95% of serotonin is produced in the gut. During perimenopause, tryptophan metabolism shifts from serotonin toward kynurenine, contributing to brain fog and mood instability (Chen et al., 2025; Epperson et al., 2011).
Fig. 2: 95% of serotonin is produced in the gut. During perimenopause, tryptophan metabolism shifts from serotonin toward kynurenine, contributing to brain fog and mood instability (Chen et al., 2025; Epperson et al., 2011).
Why does estrogen decline promote neuroinflammation?
When estrogen drops, microglia in the brain become more reactive, pro-inflammatory cytokines (IL-1β, IL-6, TNF-α) rise, and the blood-brain barrier weakens. The numbers tell the story: 44% of women in early perimenopause report forgetfulness, compared to 31% before perimenopause.
Estrogen is a natural anti-inflammatory in the brain. It keeps microglia (the brain’s resident immune cells) in a calm, protective state and holds pro-inflammatory cytokines in check (Vegeto et al., 2008). When estrogen falls, microglia shift into overdrive. In a mouse model of perimenopause, ovariectomy triggered increased microglia activation, especially in the hippocampus, the brain region responsible for memory and learning (Neidert et al., 2023).
There’s a structural side to this as well: estrogen helps maintain the blood-brain barrier. As levels fall, the barrier becomes more permeable, letting inflammatory molecules through more easily (Mosconi et al., 2021). In a study of 16,065 women aged 40 to 55, 44% of those in early perimenopause reported forgetfulness, compared to 31% of premenopausal women (Weber et al., 2021).
And here the circle closes back to the gut. Rising intestinal permeability (“leaky gut”) during perimenopause means more bacterial endotoxins make it into the bloodstream, driving systemic inflammation that worsens neuroinflammation in the brain. Vieira and colleagues (2020) published the first human study showing a menopausal increase in gut permeability, pointing to declining estrogen as the factor that downregulates tight junction proteins in the gut lining.
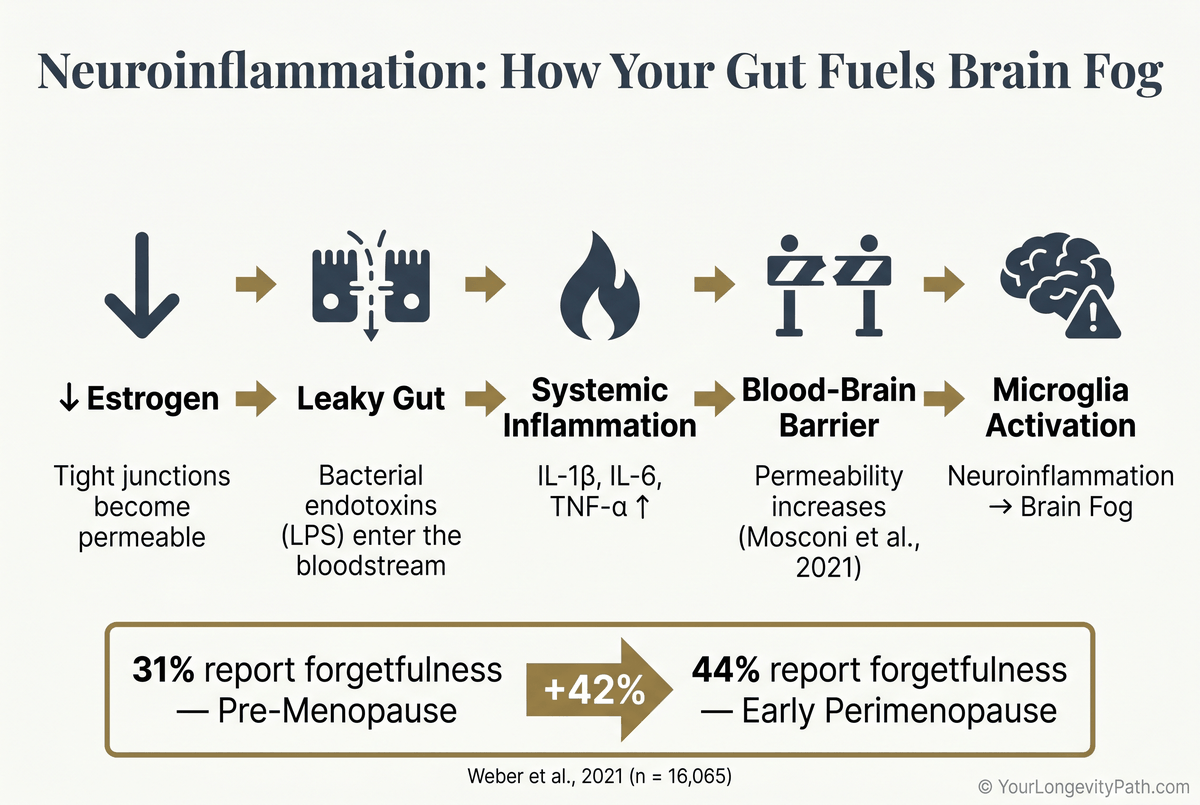 Fig. 3: The neuroinflammation cascade: from declining estrogen through leaky gut and LPS to microglia activation in the brain. 44% of women in early perimenopause report forgetfulness (Weber et al., 2021; Mosconi et al., 2021).
Fig. 3: The neuroinflammation cascade: from declining estrogen through leaky gut and LPS to microglia activation in the brain. 44% of women in early perimenopause report forgetfulness (Weber et al., 2021; Mosconi et al., 2021).
What can you do for your gut during perimenopause?
The right foods, prebiotic fiber, and cutting back on pro-inflammatory triggers can stabilize microbial diversity and support estrogen recycling through the estrobolome. Regular movement and intentional stress management add another layer of protection via the gut-brain axis.
Feed your microbiome. Fermented foods like sauerkraut, kimchi, kefir, and miso deliver live bacterial cultures. Prebiotic fiber feeds the bacteria you already have. The goal isn’t one magic superfood, it’s variety. Cruciferous vegetables (broccoli, cauliflower) and flaxseed are especially valuable for the estrobolome.
Cut pro-inflammatory foods. Ultra-processed foods, sugar, and alcohol feed inflammatory bacteria and can increase intestinal permeability. During perimenopause, when the gut barrier is already more vulnerable, this matters more than ever.
Get enough omega-3s. EPA and DHA from fatty fish or algae oil are anti-inflammatory and support both the gut barrier and neuroinflammation control.
Move regularly. Moderate exercise increases microbial diversity and supports the gut-brain axis. 150 minutes per week is a solid target.
Prioritize sleep. During deep sleep, the brain’s glymphatic system flushes out inflammatory waste products that build up during the day (Xie et al., 2013). Poor sleep keeps microglia in a reactive state and directly worsens brain fog. Seven to eight hours of quality sleep is one of the most underrated levers during perimenopause.
Manage stress. Chronic stress damages gut permeability directly via the HPA axis. Breathwork, time in nature, and consistent sleep routines help on both fronts: gut health and neuroinflammation.
Three levers working together
Brain fog during perimenopause isn’t one symptom with one cause. It shows up where three systems struggle at the same time: estrogen recycling via the estrobolome, serotonin production via the gut-brain axis, and inflammation control via microglia and the gut barrier. All three start in the gut.
You can put these first steps into practice today. But if you want to find out which levers would make the biggest difference for you personally (lab values, microbiome profile, a strategy tailored to your situation), a systematic approach pays off. That’s exactly what we cover in a free discovery call.
Scientific Sources
- Baker, J.M. et al. (2017). Estrogen–gut microbiome axis: Physiological and clinical implications. Maturitas, 103, 45–53. doi: 10.1016/j.maturitas.2017.06.025
- Peters, B.A. et al. (2022). Menopause Is Associated with an Altered Gut Microbiome and Estrobolome, with Implications for Adverse Cardiometabolic Risk. mSystems, 7(3), e00273-22. doi: 10.1128/msystems.00273-22
- Vegeto, E. et al. (2008). Estrogen anti-inflammatory activity in brain: a therapeutic opportunity for menopause and neurodegenerative diseases. Front Neuroendocrinol, 29(4), 507–519. doi: 10.1016/j.yfrne.2008.04.001
- Mosconi, L. et al. (2021). Menopause impacts human brain structure, connectivity, energy metabolism, and amyloid-beta deposition. Sci Rep, 11, 10867. doi: 10.1038/s41598-021-90084-y
- Neidert, L.E. et al. (2023). Hippocampal glial inflammatory markers are differentially altered in a novel mouse model of perimenopausal cerebral amyloid angiopathy. Front Aging Neurosci, 15, 1280218. doi: 10.3389/fnagi.2023.1280218
- Vieira, A.T. et al. (2020). Gut permeability, inflammation, and bone density across the menopause transition. JCI Insight, 5(3), e134092. doi: 10.1172/jci.insight.134092
- Epperson, C.N. et al. (2011). Interactive effects of estrogen and serotonin on brain activation during working memory and affective processing in menopausal women. Psychoneuroendocrinology, 37(3), 372–382. doi: 10.1016/j.psyneuen.2011.07.007
- Weber, M.T. et al. (2021). Menopause and cognitive impairment: A narrative review of current knowledge. World J Psychiatry, 11(8), 412–428. doi: 10.5498/wjp.v11.i8.412
- Chen, Y. et al. (2025). Mechanism of Microbiota-Gut-Brain in Perimenopausal Depression: An Inflammatory Perspective. Front Endocrinol, 16, 1578618. doi: 10.3389/fendo.2025.1578618
- Li, Y. et al. (2025). Gut microbiota has the potential to improve health of menopausal women by regulating estrogen. Front Endocrinol, 16, 1562332. doi: 10.3389/fendo.2025.1562332
- Xie, L. et al. (2013). Sleep drives metabolite clearance from the adult brain. Science, 342(6156), 373–377. doi: 10.1126/science.1241224
What causes brain fog during perimenopause?
Perimenopausal brain fog has three interconnected root causes: a disrupted estrobolome in the gut (less estrogen recycling), neuroinflammation as the brain loses estrogen's protective effect, and impaired serotonin production via the gut-brain axis.
What is the estrobolome and why does it matter during menopause?
The estrobolome is a group of gut bacteria that produce the enzyme β-glucuronidase, which reactivates used-up estrogen so it can re-enter the bloodstream. During perimenopause, microbial diversity drops, less estrogen gets recycled, and a vicious cycle sets in.
How does the gut contribute to fatigue during perimenopause?
95% of your body's serotonin is made in the gut. During perimenopause, microbiome diversity drops and tryptophan-to-serotonin conversion suffers. At the same time, intestinal permeability increases, fueling inflammation that makes fatigue worse.
This article is for informational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you have health concerns, please consult a qualified healthcare professional.